|
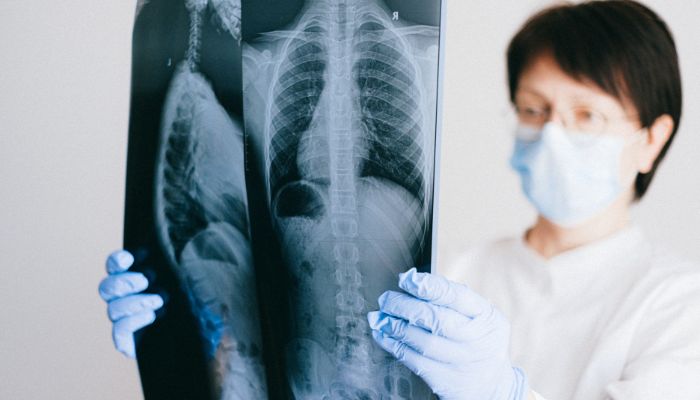
Study targets correlations among SSc patients with different types of lung disease by Andrea Lobo, PhD The degree of skin tightening is associated with changed levels of proteins implicated in inflammation and cell death among systemic sclerosis (SSc) patients with pulmonary involvement, a study in India reports.
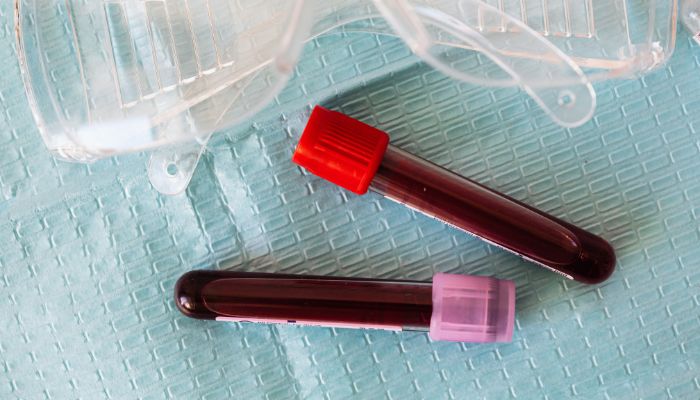
The study established protein correlations among SSc patients with different types of lung disease, which might contribute to identifying lung involvement in people with newly diagnosed SSc, the team suggested. “A longitudinal follow up in these patients with assessment of these immunological parameters may be helpful in monitoring the disease,” the researchers wrote. The study, “A comparative study of modulatory interaction between cytokines and apoptotic proteins among Scleroderma patients with and without pulmonary involvement,” was published in the journal Cytokine. SSc is characterized by abnormal scarring of the skin and potentially internal organs, such as the heart, kidney, lungs, and digestive tract. The disease is thought to develop from the combination of immune dysfunction — meaning the activation and recruitment of immune cells and the production of self-targeting antibodies (fibrosis) — and damage to small blood vessels. The most prominent forms of lung involvement in SSc are interstitial lung disease (ILD), a group of conditions characterized by lung inflammation and fibrosis, and pulmonary arterial hypertension (PAH), caused by the narrowing of small blood vessels that transport blood to the lungs. Studies have reported the involvement of proinflammatory and pro-fibrotic signaling molecules called cytokines in SSc. Also implicated in the disease are proteins associated with apoptosis — programmed cell death (as opposed to cell death caused by injury), which can alter immune responses. To investigate the possible correlation between blood cytokines and apoptotic proteins in SSc, researchers in India analyzed 100 treatment-naïve SSc patients, with or without pulmonary involvement, as well as 100 healthy people who served as controls. Levels may serve as biomarkers for the disease, help predict outcomes by Steve Bryson, PhD Levels of microparticles, tiny molecule-filled sacs shed from cells, were altered in the bloodstream of adults with systemic sclerosis (SSc), a study reports.
Elevated microparticles derived from blood-clotting platelets were associated with disease-related antibodies and longer disease duration. By contrast, lower levels of microparticles shed from endothelial cells that line blood vessels were tied to worse skin and blood vessel involvement. These results suggest microparticles may participate in developing SSc and serve as biomarkers to predict outcomes, the researchers noted in “Microparticles: potential new contributors to the pathogenesis of systemic sclerosis?” which was published in Advances in Rheumatology. SSc, also called scleroderma, is an autoimmune disease that may affect multiple systems in the body. It’s marked by scar tissue building up in the skin and/or several organs, such as the heart, lungs, kidney, and digestive tract. Microparticles (MPs), or microvesicles, are tiny membrane-bound sacs shed from cells undergoing activation or apoptosis (programmed cell death), which contain cell type-specific components. Mostly shed from platelets, white blood cells, and endothelial cells, MPs have been shown to modulate inflammatory and blood clotting activities. Studies have suggested that people with SSc have higher levels of MPs in their blood, particularly those derived from endothelial cells (EMPs) and platelets (PMPs). A columnist praises her husband's approach to being a spouse caregiver by Lisa Weber We toasted to 18 years as a married couple while looking out over Tampa Bay, Florida. My amazing husband, Ross, had planned out every detail, from the surprise dinner reservations in the city to the romantic sunset-watching at the park. If you know me, you know pulling off a surprise is nearly impossible. Ross endured a week of grilling questions and still kept the itinerary under lock and key.
Although it was a beautiful night, we had to accommodate my blue-toned hands, a result of Raynaud’s, and sit indoors. But we moved forward with the evening and didn’t pay my disease much attention. And even when my gastroparesis limited my options on the menu, we chose to ignore it for the night and focus only on the happy memories we’ve built together. I even drank wine without worrying about the insufferable inflammation it would cause the next day. Because every now and then, it helps to take a vacation day from scleroderma. Study to focus on how immune system responses drive rare disease by Lindsey Shapiro, PhD The National Scleroderma Foundation has awarded a $200,000 research grant to a University of Minnesota scientist to study how immune system responses drive the emergence of scleroderma — the cause of which remains unknown. The funding for researcher Rafael Contreras-Galindo, PhD, comes in the form of the two-year Marta Marx Fund for the Eradication of Scleroderma Award, given to scientists submitting the second-highest scoring research proposal to the foundation each year. The project will be titled, “Centromeres, Chromosome Instability and cGAS-STING Activation in Scleroderma Fibrosis.” “Identifying the cause of scleroderma is the main goal of this study,” Contreras-Galindo, assistant professor at the University of Minnesota’s The Hormel Institute, said in a university press release. Scleroderma is an autoimmune disease that arises when the body’s immune system becomes overactive and attacks its own tissues, in this case, causing inflammation and damage to connective tissue. In response, the cells overproduce collagen — a connective tissue protein — leading to scar tissue buildup that hardens and tightens connective tissues in the skin or other organs. While the results are known, the mechanisms underlying this process haven’t been fully worked out. Contreras-Galindo’s team will specifically examine the potential role of centromere dysfunction in triggering these harmful immune responses. Chromosomes, thread-like structures where DNA is packaged, consist of two identical halves. When a cell divides and replicates, these two halves split apart, ensuring that each new cell has the same genetic information as its parent. Centromeres sit between these two halves, holding them together and facilitating their split during cell division. If that process is defective, chromosomes become unstable and certain immune pathways can be triggered in response. With his team, Contreras-Galindo found that people with scleroderma had signs of centromere defects in their skin cells not seen in healthy people. Findings from their work were published in a study in the journal Nature Communications Data also indicated that an immune pathway called cGAS-STING was activated in SSc cells, which the researchers believe was triggered by the chromosomal abnormalities that were found. Joint pain common in pediatric scleroderma patients, lung disease in older ones by Lindsey Shapiro, PhD The clinical presentation of systemic sclerosis (SSc) differs significantly between adult and pediatric patients, according to a recent study in Turkey.
Particularly, adults were more likely to have lung disease and to be at a higher risk of death than children, who were more likely to experience joint inflammation and pain. These differences, in turn, influenced treatment choices, which diverged significantly between adults and children. The study, “Juvenile and adult-onset scleroderma: Different clinical phenotypes,” was published in the journal Seminars in Arthritis and Rheumatism. Dr. Lee Shapiro, CMO of the Steffens Scleroderma Foundation, shares his insight by Amy Gietzen of Scleroderma News In 2018, I was asked to be a keynote speaker at an interprofessional education event (IPE) that aimed to educate graduate students in various healthcare disciplines about scleroderma. I’m a patient advocate who’s lived with the disease for more than two decades, and I pride myself on spreading awareness and educating the public, so I gladly accepted. The event was sponsored in part by the Steffens Scleroderma Foundation, a nonprofit whose mission is to support research toward the treatment and cure of scleroderma and to promote greater understanding of the disease, especially among healthcare professionals. It’s also where I met Dr. Lee Shapiro, a prominent rheumatologist and the foundation’s chief medical officer. I’ve long admired Shapiro’s passion and dedication to the scleroderma community, so I recently reached out to him via email for an interview. Excerpts of our conversation follow, with light editing for clarity. Dr. Lee Shapiro, chief medical officer and founder of the Steffens Scleroderma Foundation. (Courtesy of Lee Shapiro)
Study probes autoimmunity link between SSc and primary biliary cholangitis by Andrea Lobo, PhD Systemic sclerosis (SSc) patients with primary biliary cholangitis (PBC), a disease that causes inflammation and scarring of the liver bile ducts, have milder symptoms that rarely lead to major complications, compared to patients with SSc alone.
A study with that finding also determined SSc-only patients had a higher incidence of heart and pulmonary diseases at follow-up, as well as new digital ulcers, than those with SSc and PBC. Autoimmunity may be a link between SSc and PBC, and patients with both conditions “may be considered a real crossroad of polyautoimmunity that seem to alleviate the SSc phenotype [characteristics],” the researchers wrote. The study, “Systemic sclerosis and primary biliary cholangitis: Longitudinal data to determine the outcomes,” was published in the Journal of Scleroderma and Related Disorders. SSc is caused by activation of the immune system, leading to inflammation and accumulation of scar tissue (fibrosis) in the skin and internal organs. Also called scleroderma, SSc has been associated with other autoimmune diseases, such as PBC. PBC-specific autoantibodies — meaning those attacking the body’s own tissues — have been associated with higher mortality. The prevalence of PBC in SSc patients is estimated to be 2-3% higher than in the general population. But PBC-specific autoantibodies are even more frequent. The condition is more frequent in people with limited SSc, characterized by skin symptoms in the face, arms, hands, and fingers, and has been suggested to identify SSc patients with milder body-wide disease. Elevated levels tied to more severe interstitial lung disease by Patricia Inácio, PhD Elevated blood levels of the cold-inducible RNA-binding protein (CIRP) are linked with more severe interstitial lung disease (ILD) in systemic sclerosis (SSc) patients and may be a marker of disease activity, a study from Japan reports.
“Our results suggest that serum [blood] CIRP levels may serve as a useful serological marker of SSc-ILD in terms of disease activity and therapeutic effects,” the researchers wrote. These findings “hold the potential to pave the way for a novel design for the treatment of patients with SSc-ILD.” The study, “Serum cold-inducible RNA-binding protein levels as a potential biomarker for systemic sclerosis-associated interstitial lung disease,” was published in the journal Scientific Reports Protein’s levels a potential blood marker of SSc-ILD progression ILD comprises a group of lung disorders marked by inflammation and fibrosis (scarring) that causes lung tissue to thicken and stiffen, restricting the volume of air that enters and leaves the lungs. While blood biomarkers have been proposed, “few of them could help estimate the progression of SSc-ILD,” the researchers wrote. Cells in damaged tissues release warning signaling molecules — called damage-associated molecular patterns (DAMPs) — as a way of alerting and activating the immune system. Several DAMPs have been reported to be involved in SSc. The CIRP protein, recently identified as a DAMP, has rising levels following exposure to stressors such as low oxygen levels, UV radiation, and glucose (sugar) deprivation. CIRP, a “general stress-response protein,” is found in several tissues, including the skin, lungs, and heart. While the protein recently was implicated in the development of idiopathic pulmonary fibrosis, its role in SSc is not well known. Findings: Education, marital status may affect symptoms by Margarida Maia, PhD Having a higher level of education or being married may mean fewer symptoms of depression for people with systemic sclerosis (SSc), according to a systematic review of multiple studies.
Researchers also observed that lung involvement, breathing problems, and tender joints were linked to more symptoms of depression, but not anxiety. Because there was not much evidence available, “future studies should examine prevalence of mood and anxiety disorders in SSc in large, representative samples,” the researchers wrote. The systematic review, “Results from a living systematic review of the prevalence of mood and anxiety disorders and factors associated with symptoms in systemic sclerosis,” was published in the journal Scientific Reports. People with SSc experience a wide range of symptoms caused by a buildup of scar tissue in the skin and possibly internal organs such as the heart, lungs, kidneys, and intestinal tract. “Disease presentation is extremely heterogeneous, and its course is unpredictable,” the researchers wrote. Because they are unsure of how their disease will progress, many people with SSc experience changes in mood or begin to feel anxious. Also contributing to mood and anxiety disorders are “high levels of chronic pain, fatigue, body-image distress, overall disability, increased risk of mortality, and limited treatment options,” the scientists added. Patients positive for Scl-70 antibodies at more risk of major organ involvement by Steve Bryson, PhD People with systemic sclerosis (SSc) who test positive for Scl-70 self-reactive antibodies are at a higher risk of major organ involvement, particularly the lungs, than those with other types of autoantibodies, a study suggested.
Digestive tract involvement was associated with the presence of anti-nuclear (ANA) autoantibodies. SSc patients with Scl-70 autoantibodies should be monitored for lung disease, regardless of whether their disease is limited to the skin or occurs in both skin and internal organs, the researchers recommended. “Understanding these risk factors might help with earlier diagnosis and better disease management for people with SSc,” they noted in the autoantibody study, “Clinical phenotype in scleroderma patients based on autoantibodies,” which was published in Rheumatology Advances in Practice. SSc, also called scleroderma, is an autoimmune disease that features the buildup of scar tissue in the skin and several other organs, potentially. It’s usually classified into two subtypes, based on the extent of skin symptoms. Limited cutaneous SSc (lcSSc) is indicated by skin symptoms confined to the face and arms below the elbows. Diffuse cutaneous SSc (dcSSc) involves widespread skin scarring that’s accompanied by internal organ damage. “However, dividing SSc according to skin involvement might be too simplistic, meaning that we could overlook a wider spectrum of the disease,” the researchers wrote. People with SSc have self-reactive autoantibodies that mistakenly target cellular components in their own tissues, including Scl-70, ANA, and anti-centromere (ACA) autoantibodies. While lcSSc has been associated with anti-ACA autoantibodies and dcSSc with anti-Scl-70 autoantibodies, some people with lcSSc are positive for Scl-70 autoantibodies and some with dsSSc are positive for ACA autoantibodies. |
AuthorScleroderma Queensland Support Group Archives
April 2024
Categories
All
|
Scleroderma Association of Queensland
©Scleroderma Association of Queensland. All rights reserved. Website by Grey and Grey.