|
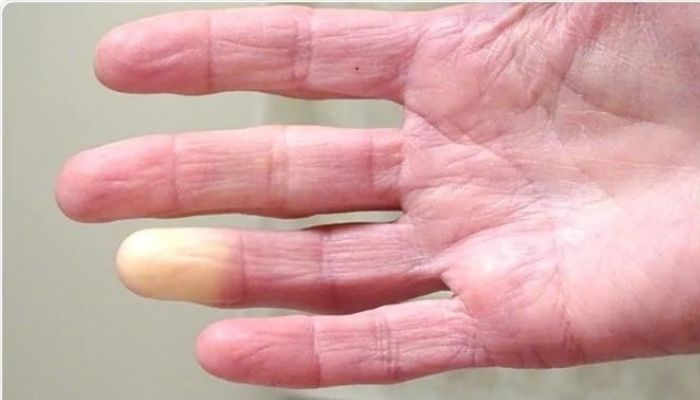
A Canadian advocate tells how she's managed the disease over the years - Article from Scleroderma News  Silvia Petrozza is a powerhouse! Known as the Autoimmune Slayer, she has almost 1,700 Instagram followers and always seems to have her fingers in disease advocacy efforts in Canada. A mother of three, she also has her own business — impressive for a woman living with scleroderma since age 23. I interviewed her by email. Following are her responses, lightly edited for clarity. AG: Tell me about your journey to diagnosis. SP: When I was a teenager, I unknowingly experienced Raynaud’s syndrome. My doctor chalked it up to poor circulation. However, periodically throughout my teenage years, I was sick. But my doctor never really looked into why. In 2007, within months of having my first child, I was officially diagnosed with scleroderma. My Raynaud’s started progressing rapidly, and the pain became unbearable. I even experienced my first digital ulcer. My sister had been convinced I had lupus. However, after my initial doctor visit, scleroderma was the verdict. I immediately began looking for a specialist, which turned into a long and draining process. Because scleroderma is so rare, I had to travel quite a ways, to Toronto, for adequate care. How difficult has it been living with scleroderma? Living with scleroderma is hard! I’ve had to find my “new normal” in order to cope with daily life. Scleroderma can also be unpredictable. Tasks like getting dressed, doing chores, and being a mom can be very difficult. I’ve had to learn to adjust my expectations. I’ll have days when my pain is manageable. But in order to maintain my status quo, I undergo monthly scheduled infusions of iloprost (synthetic prostacyclin, known by the brand name Ventavis and often used for pulmonary arterial hypertension). These treatments require me to leave my family, travel two hours from home, and then spend two days in bed recovering. Scleroderma doesn’t just affect me, but my family as well. Columnist Amy Baker from Scleroderma News explains how she maintains a positive attitude Living with a chronic illness like scleroderma can be a constant challenge. Dealing with myriad doctor appointments, pharmacy runs, and symptoms is often time-consuming. Staying calm while managing this disease is easier said than done.
One thing that’s helped me on this crazy journey is maintaining a positive attitude. But how can someone be positive while living with such a difficult illness? One way is to realize that not every day is a bad day. Some days, there are no appointments. Some days, I feel like my old self. And on the days that are hard, I listen to some uplifting music, feed my soul, and do what makes me feel good. Following are a few ways I find my Zen while living with scleroderma. Overwhelmed Columnist Amy Gietzen struggles with a slew of mysterious symptoms A chronic, life-threatening health problem can disrupt all aspects of your life, especially when it develops unexpectedly.
When I was diagnosed with scleroderma at age 19, I was overwhelmed by difficult emotions, from fear and worry to profound sadness, despair, and grief. These feelings rushed over me like cold waves of water, leaving me numb and frozen with shock. I felt like I’d never be able to cope. For years I put on a brave face. I put my head down and did the work, always trying to be proactive and positive in the face of scleroderma. But I still felt like I was moving further and further away from my goal of stabilizing my symptoms. When would all of my hard work, dedication, and treatment compliance pay off? Body betrayal is a common experience among people with chronic illness by Amy Gietzen from Scleroderma News After I was diagnosed with scleroderma in 2001, I found myself having some strange thoughts, such as, “What’s wrong with me? My body hates me. I hate my body. What did I do to deserve this? Why can’t I just be normal again?”
While many of the feelings I experienced are hard to describe and identify, I vividly remember the feeling of betrayal coursing through my veins for months after my diagnosis. Because scleroderma can affect people in so many different ways, and because symptoms can ebb and flow and change over time, it can be easy to think that your body is out to get you. For me, it felt like my body was betraying my trust in it. I can’t recall a time since my diagnosis that I wasn’t in pain or, at the very least, uncomfortable with the changes I was experiencing. In my first few years with scleroderma, I felt like I had no control over what was happening to me. At any given time, my hands would cramp, my muscles would stiffen and tense, and my skin would itch so intensely that I needed to ice it with cold packs. HSI technology seen as novel way to quantify disease activity by Andrea Lobo, PhD from Scleroderma News Hyperspectral imaging (HSI) — technology used in medicine to obtain a three-dimensional dataset — may be a feasible, non-invasive technique to quantify the severity of Raynaud’s phenomenon associated with systemic sclerosis (SSc-RP), according to a new study.
This “technology may present a novel, fast, and effective method to quantify and monitor disease activity in SSc-RP,” the researchers wrote. HSI technology also may provide needed outcome measures for clinical trials of potential treatments for the condition. “There is an unmet medical need to enhance the SSc-RP clinical trial design to enable valid testing of therapy,” the team wrote. The study, “Hyperspectral imaging in systemic sclerosis-associated Raynaud phenomenon,” was published in the journal Arthritis Research & Therapy. Findings in Phase 2 trial of prednisolone seen as inconclusive due to pandemic by Patricia Inácio, PhD from Scleroderma News Moderate doses of oral prednisolone, a corticosteroid, given for a short period may help to ease symptoms in people with early diffuse cutaneous scleroderma (dcSSc), a Phase 2 trial suggests. The study, intended to assess whether moderate dose of corticosteroids are safe and effective for early dcSSc, was affected by the COVID-19 pandemic starting in March 2020 and failed to provide conclusive results, its researchers noted. Given the disease’s “inflammatory basis,” however, its findings may provide “support for the view of many clinicians that it is not unreasonable to prescribe short-term moderate dose prednisolone for symptom control, always remembering the importance of careful monitoring of blood pressure and renal function,” the team wrote. The study, “A Phase II randomised controlled trial of oral prednisolone in early diffuse cutaneous systemic sclerosis (PRedSS)” was published in the journal Rheumatology. Prednisolone use ‘contentious’ due to risk of renal crisis with dcSSc Scleroderma, also known as systemic sclerosis (SSc), is marked by progressive scarring in the skin and, possibly, internal organs that include the kidneys. The disease is caused by a wrongful immune response against the body’s own proteins. Organ damage is a particular risk for people with dcSSc, and one that develops early in the disease’s course and can worsen quickly. Currently, no effective disease modifying treatments are available for these patients. Although the inflammatory basis of dcSSC supports the use of corticosteroids, their use poses of risk of a renal, or kidney, crisis. “Whether or not they should be prescribed is therefore highly contentious,” the researchers wrote. Scientists in the U.K. designed the Phase 2 PRednisolone in early diffuse SSc (PRedSS) trial (NCT03708718) to assess the safety and effectiveness of prednisolone at a moderate dose compared to a placebo in adults with early dcSSc. The study was funded by Versus Arthritis. |
AuthorScleroderma Queensland Support Group Archives
July 2024
Categories
All
|
Scleroderma Association of Queensland
©Scleroderma Association of Queensland. All rights reserved. Website by Grey and Grey.